Most patients present with pain, swelling and difficulty with shoewear. All patients should be asked about possible underlying causes of chronic infection, such as diabetes and steroid use.
The foot should be examined for mechanical factors which might precipitate nail pressure or infection. Inspect the shoes – they may be the main source of pressure. Look for tenderness in the pulp or proximally, which may indicate osteomyelitis.
Differential diagnosis includes subungual exostosis, primary osteomyelitis of the phalanx and tumours of the nail bed, including subungual melanoma.
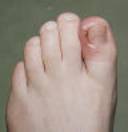
An ingrown nail affecting the fibular sulcus of the left hallux
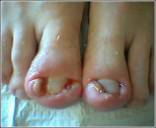
A longstanding presentation affecting both sulci of both hallux nails
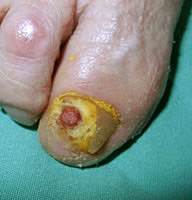
Subungual exostosis
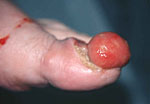
Acral lentiginous melanoma
Classification
There is no consensus on the classification of the lesion at presentation. The most frequent classification quoted in the literature is that first proposed by Heifetz (1937) and subsequently used by Mogensen (1971).
- Grade 1: Pain, reddening and slight swelling of the nail sulcus.
- Grade 2: As above, accompanied by infection and suppuration.
- Grade 3: As above with the formation of granulation tissue (sometimes referred to as hypergranulation tissue.
Infection and suppuration is more marked in grade 3. Untreated ingrown toenails can have serious and limb threatening consequences. Cox and Jones (1995) reported development of osteomyelitis as a consequence of chronic ingrown toenails. Tumours, primary or metastatic, can mimic the presentation of an ingrown toenail (Goldenhersh 1992, Requena 1993, Lemont 2002).
