Investigations will be described in terms of what issue they are intended to clarify.
Assess diabetic status and metabolic effects
Review the patient's diabetic control records. A finger-stab BM test will estimate blood glucose; a random blood sample for glucose measurement is more accurate. The glycosylated haemoglobin test (HbA1C) summates blood glucose control over the last few months. The upper limit of normal is about 6.5% and risk increases with glycosylation, particularly above 8.5%.
Blood urea and electrolytes assess renal function and may indicate potassium or sodium depletion secondary to medication. Unless the patient is clinically ill further tests are not usually required.
Assess deformity
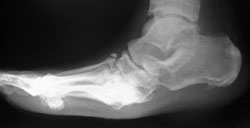
Standing lateral radiograph shows rocker-bottom midfoot deformity with equinus
Diabetic foot deformities, especially after Charcot arthropathy, are complex in three dimensions. Standing radiographs relevant to the site of deformity give a helpful indication and allow assessment of bone stock. In the hindfoot and midfoot we use a "deformity series":
- standing hindfoot alignment view modified from Saltzman and el-Khoury (1995)
- standing lateral view
- standing dorsoplantar view
plus an oblique view.
In very complex deformities, especially in the hind and midfoot, a CT can give useful additional information.
Diagnose infection
The International Working Group on the Diabetic Foot have published guidelines on the diagnosis and management of infection (Peters 2013) and these are largely reflected in the NICE guideline (NICE 2011). Markanday (2014) reviewed the evidence helpfully in the course of proposing a score-based approachto evaluating the probability of infection.
Routine white cell count, ESR and CRP can show evidence of infection, but may be normal or there may be other possible explanations of abnormal tests. ESR >70mm/hr strongly suggests osteomyelitis (Butalia 2008). Increased CRP may be less specific for bony versus soft tissue infection (Markanday 2014)and the value of procalcitonin is not yet clear (Muluoglu 2011). Diabetic control generally deteriorates in the presence of infection.
Plain radiographs may show bone erosion, porosis, new bone formation or changes of chronic osteomyelitis. However, they may be negative in the presence of infection. Isotope bone scanning is fairly sensitive for infection but not very specific; other nuclear medicine techniques such as indium scanning or labelled white cell scanning are somewhat more accurate but still not specific enough.
MRI and PET scanning with fluorodeoxyglucose have emerged as the imaging techniques of choice over the last few years (Peters 2013, Markanday 2014). PET scanning obviously has an advantage where metal implants are in place, but MRI is generally more available and comparative studies have not shown a clear advantage for either technique.
Diagnose Charcot arthropathy
Plain radiographs will show abnormalities in stages 1-3 of Charcot: initially fragmentation, bone lysis, fractures and dislocations, followed by coalescence, healing and remodelling. However plain radiographs may be normal in the presnce of a hot swollen foot (stage 0). In this situation nuclear medicine tests will show markedly increased uptake, and MRI shows bone oedema and stress fractures (Chantelau 2005). There is interest in using MRI earlier to diagnose stage 0 Charcot, as the results of treatment in this stage are better (Chantelau 2013, Wukich 2011).
Charcot versus infection
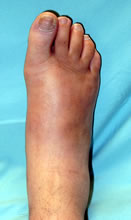
Acute hot diabetic foot - Charcot or infection? No ulcer so Charcot is far more likely (it was Charcot)
This is a significant clinical dilemma. Patients with Charcot arthropathy have often been treated for infection. Ertugrul (2013) offers a useful review.
Diabetic control may be poor in both scenarios, and both body temperature and local foot temperature may be raised, as is the CRP. Almost all diabetic foot infections follow ulceration (198/199 infections in the seried of Lavery (2006)).
Plain radiographic features can be similar in both, especially early in the clinical course. Fragmentation and dislocation are in favour of Charcot but do not rule out infection. Nuclear medicine studies show abnormal increased uptake in both situations.
MRI shows early fractures, feagmentation and extensive bone oedema in Charcot which strengthen the case against infection.
A warm swollen foot without an ulcer is usually Charcot; MR may help strengthen the clinical impression but is not usually necessary. Infection is more likley in the presence of an ulcer, especially in the presence of a positive probe-to-bone test. PET or MR scanning may be useful but the gold standard for diagnosis of infection is bone biopsy (Zuluaga 2005, O'Meara 2006, Ertugrul 2013). Expert clinical judgement is required to integrate clinical, imaging and laboratory findings.
